How to Identify a Bone Fracture Early
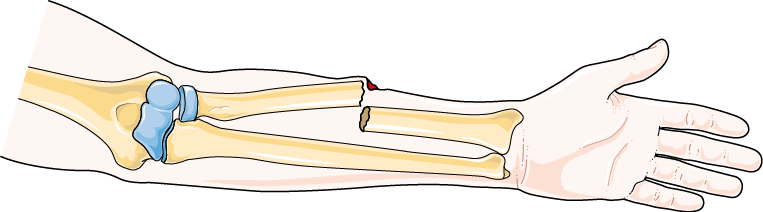
Bone fractures are among the most common injuries worldwide. Early identification of a fracture dramatically improves treatment outcomes. Many patients delay seeking care due to uncertainty about their injury. Understanding the early signs of a fracture is critical knowledge. Some fractures are obvious, while others are surprisingly subtle. Learning how to recognize fractures early can prevent serious complications. This guide explores key signs, symptoms, and identification strategies.
What Happens to Bone During a Fracture
A fracture occurs when force exceeds the bone's structural strength. The bone cracks, breaks, or shatters depending on force intensity. Surrounding tissues, including muscles and blood vessels, are also affected. Nerves near the fracture site may become compressed or stretched. Blood vessels bleed into the surrounding tissue, causing bruising. This tissue response is what generates the familiar pain and swelling. Understanding the mechanics helps explain the symptoms patients experience.
Fractures are classified by type, pattern, and severity. Transverse fractures run horizontally across the bone shaft. Oblique fractures occur diagonally and may be unstable. Spiral fractures result from twisting forces on the bone. Comminuted fractures shatter bone into multiple fragments. Stress fractures develop gradually from repetitive loading. Greenstick fractures occur in children whose bones are more flexible. Each fracture type presents with slightly different early signs.
Classic Signs and Symptoms of a Fracture
Recognizing the classic signs of a fracture is the first step. Pain is the most immediate and universal symptom after injury. The pain is typically sharp and worsens with movement or pressure. Swelling begins within minutes of the injury occurring. Bruising, or ecchymosis, develops as blood spreads beneath the skin. Deformity may be visible if bones are significantly displaced. Tenderness at a specific point along the bone is characteristic. Difficulty bearing weight or using the injured limb is common.
Pain Characteristics That Suggest Fracture
Fracture pain has specific characteristics that distinguish it. Point tenderness directly over the bone is highly indicative. Pressing gently on the injury site causes sharp, localized pain. Pain that is diffuse and widespread may suggest soft tissue injury instead. Bony tenderness along the length of the bone is significant. The Ottawa Ankle Rules and Ottawa Knee Rules guide clinical assessment. These validated clinical tools help determine whether imaging is needed. Physicians rely on these decision tools to avoid unnecessary X-rays efficiently.
The Role of Swelling and Bruising in Identification
Swelling after an injury is a nonspecific but important sign. It begins immediately as the body's inflammatory response activates. Fracture-related swelling tends to be more severe and localized. It often feels firmer than soft tissue swelling from a sprain. Bruising typically appears hours after the initial injury occurs. Its location may shift as blood tracks through tissue planes. Bruising directly over a bony prominence strongly suggests fracture. Severe bruising early after injury is a warning sign worth investigating.
Recognizing Subtle and Stress Fractures
Not all fractures present with obvious, immediate symptoms. Stress fractures develop gradually from repetitive mechanical loading. Runners, dancers, and military recruits are commonly affected populations. The pain starts as a dull ache during activity and improves at rest. Over time, the pain begins earlier during activity and worsens. Eventually, pain may persist even during rest and at night. Localized tenderness over a specific bone area is characteristic. The hop test, where hopping on the affected foot causes pain, is useful.
Clinical Tests Used for Fracture Identification
Clinicians use several physical examination tests to identify fractures. The fulcrum test applies bending force along a long bone. Pain provoked by this test suggests a stress fracture. Vibration testing uses a tuning fork placed near the injury site. Vibration transmitted through a fractured bone increases pain. The squeeze test applied to the forearm or leg detects shaft fractures. These clinical assessments guide decisions about imaging investigations. No single test is definitive, so combining findings improves accuracy.
Imaging Techniques for Confirming Early Fractures
Physical examination alone cannot always confirm a fracture. Imaging studies provide definitive confirmation in most cases. X-rays are the first-line imaging modality for suspected fractures. They detect most complete fractures and significant bone injuries. However, early stress fractures and nondisplaced fractures may be missed. MRI is the gold standard for detecting early stress fractures. It shows bone marrow edema before fracture lines are visible. CT scans evaluate complex fractures in multiple planes clearly. Bone scans detect areas of increased metabolic activity related to fracture.
Early imaging prevents delays in diagnosis and fracture treatment, which is essential for recovery. Delayed diagnosis allows fractures to displace or worsen unnecessarily. Early immobilization and treatment significantly improve long-term outcomes. Prompt imaging after a suspected injury is always the right decision.
When to Seek Immediate Medical Evaluation
Certain signs indicate that a fracture requires urgent medical attention. Severe deformity of a limb demands immediate emergency care. Open fractures, where bone protrudes through skin, are medical emergencies. Loss of sensation or movement distal to the injury site is critical. Pallor, coolness, or absence of pulse distal to the fracture is serious. These neurovascular compromise signs require urgent evaluation and intervention. Any suspected fracture in a child warrants prompt professional assessment. When in doubt, always seek medical evaluation rather than waiting at home.
Special Populations and Fracture Identification
Certain populations are at higher risk for fractures generally. Elderly individuals with osteoporosis fracture with minimal trauma. A simple fall from standing height can cause severe fractures. Hip and vertebral fractures in older adults are particularly dangerous. Patients on corticosteroids have significantly weakened bone structure. Children's growing bones fracture differently than adult bones do. Pathological fractures occur through bone weakened by disease or tumor. Identifying fractures in these groups requires heightened clinical awareness.
Recognizing Hip Fractures in Elderly Patients
Hip fractures in elderly patients can present subtly sometimes. The patient may recall a fall or simply be unable to stand. The affected leg often appears shortened and externally rotated. Groin pain that is worse with hip rotation is characteristic. Some patients with incomplete hip fractures can still walk. This can mask the severity of the underlying injury significantly. Any elderly patient with hip pain after a fall needs imaging. Delayed diagnosis of hip fractures leads to serious complications and mortality.
Pediatric Fracture Identification Challenges
Children's fractures present unique diagnostic challenges for clinicians. Growth plates, called physes, are the weakest part of a child's bone. Salter-Harris fractures involve the growth plate specifically. These fractures are graded by their extent and surgical implications. Greenstick fractures occur when one cortex breaks and the other bends. Children may not report pain clearly or accurately to caregivers. Tenderness, swelling, and refusal to use a limb are important clues. Parents should seek evaluation whenever a child refuses to use a limb.
Toddler's Fractures and Non-Accidental Trauma
Toddler's fractures occur from minor twisting falls in young children. They appear as subtle spiral fractures of the tibia. These fractures may not be visible on initial X-rays taken early. Repeat imaging after 7 to 10 days may reveal the fracture. Unusual fracture patterns in children raise concern for non-accidental injury. Multiple fractures of different ages are a significant warning sign. Physicians are obligated to investigate and report suspected child abuse. Early identification protects vulnerable children from ongoing harm effectively.
Preventing Missed Fractures and Delayed Diagnosis
Missed fractures are a significant source of patient harm in medicine. Clinical vigilance and proper imaging protocols reduce missed diagnoses. Follow-up X-rays after initial negative results are sometimes necessary. Clinical deterioration despite normal initial imaging warrants repeat assessment. Patients should return for evaluation if symptoms worsen over time. Second opinions are appropriate when clinical uncertainty persists. Good communication between patients and providers reduces diagnostic delays. Early and accurate fracture identification leads to better outcomes for all patients.
Recognizing a bone fracture early is a skill worth developing. It requires attention to pain, swelling, bruising, and deformity. Clinical examination and appropriate imaging confirm the diagnosis. High-risk populations require extra vigilance and lower imaging thresholds. Prompt identification leads to timely treatment and better healing outcomes. Never ignore persistent pain after an injury, as early care changes everything.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- الألعاب
- Gardening
- Health
- الرئيسية
- Literature
- Music
- Networking
- أخرى
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


